Many horse athletes develop some form of degenerative joint disease, also known as arthritis. What does a healthy joint look like and why does a joint develop arthritis? Why are hyaluronic acid (HA), MSM, glucosamine, chondroitin and collagen important in a joint?
Synovial membrane
The synovial membrane lines the joint cavity where articular cartilage is not present. It is the inner lining of the joint capsule. The 3 principal functions of the synovial membrane are:
- phagocytosis (eating up and getting rid of unwanted components)
- regulation of protein and hyaluronic acid content of the joint fluid
- regeneration
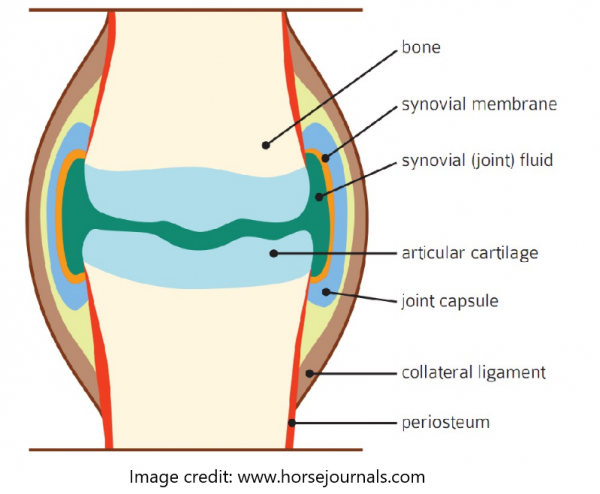
The synovial membrane acts as an important permeability barrier, which means it controls which components are allowed to enter the joint fluid, which is how the synovial membrane controls joint fluid composition.
Trauma to the joint capsule and its synovial membrane results in inflammation of these structures (called synovitis and capsulitis). This causes increased vascular permeability (the synovial membrane allows more fluid from the blood circulation to flow into the joint), and the synovial membrane’s protein production goes up. This is how synovitis causes joint effusion and pain.
The synovial membrane is an elastic structure, which is needed for joint motion and shock absorption. When the synovial membrane becomes inflamed and fibrotic (scar tissue), this results in joint stiffness and reduced shock absorption.
Synovitis also causes a release of deleterious inflammatory mediators, that can cause biochemical damage and contribute to a degenerative joint process over time (osteo-arthritis). When the synovial membrane becomes damaged it can heal with time. However, as with scar formation on skin, the resulting synovial tissue may be more fibrotic and therefore does not always have the same qualities. It might not regulate and maintain the joint and joint fluid as it normally should.
In traumatic joint effusions, there are changes in joint fluid composition. Many joint supplements and injectables are focused on creating a better joint fluid composition, that has better lubricating and protective properties.
Joint cartilage
Joint cartilage covers the bone surfaces in a joint. It is made out of chondrocytes (cartilage cells) and the extracellular “matrix” around the chondrocytes. This “matrix” contains collagen fibres, proteoglycans, glycoproteins and water.
Collagen in joint cartilage
Collagen type 2 comprises up to 95% of the collagen in articular cartilage and forms fibers that are intertwined throughout the cartilage “matrix”. Other types of collagen help support and strengthen the collagen type 2 fiber network. This intertwined network of collagen fibers is what gives the joint cartilage its stiffness and tensile strength, which is essential to its function.
Proteoglycans in joint cartilage
Proteoglycans are the other major solid component of the articular cartilage “matrix”. They occupy the spaces between the collagen fibers. Every proteoglycan unit is made up of a protein core and glycosaminoglycan (GAG) side chains. Most of the proteoglycans in cartilage form even larger units by attatching to hyaluronic acid (HA), and more than a 100 proteoglycans can attach to one HA at a time. The combined unit is called an aggrecan. Aggrecans are contained by the collagen network and give the cartilage its compressive stiffness, which has an important role in shock absorbtion.
The two major GAGs used to make a proteoglycan unit are chondroitin-6-sulphate and keratan-sulfate. For young animals chondroitin-4-sulfate is also important.
There are also other constituents of cartilage, which are not discussed here as that would probably complicate this summary too much.
Joint cartilage – nutrition and pain
Some joint supplements focus on supplying the building blocks for healthy cartilage (collagen, chondroitin, etc). Whether the body utilises these products for the intended purpose is a matter of discussion. The joint cartilage gets its nutrients from the synovial fluid, and the synovial membrane regulates synovial fluid composition. Healthy joint fluid composition will therefore aid healthy cartilage.
There are no nerves in joint cartilage. Body posture awareness and pain sensation comes from nerves in the joint capsule, synovial membrane, ligaments, muscle and the bone that’s attatched to the joint. Direct trauma to the joint cartilage and the bone underneath it can result in cartilage ulceration, fractures or cartilage loss, resulting in osteoarthritis. Recurrent fatigue damage to the collagen network (from strenuous activities) could cause a more insidious osteoarthritis process.
Joint cartilage – remodelling
Chondrocytes (cartilage cells) produce all the components of the cartilage “matrix”. Cartilage matrix is constantly degraded and simultaneously built up, a process that should be in balance. Depending on the age of the animal and the loads on the joints, the balance can be tipped a little to facilitate remodelling or growth. However, even if rebuilt, cartilage that is compromised by loss of glucosaminoglycans (GAG) or collagen is vulnerable even to normal forces.
Lubrication of joints
HA is the important component in the joint fluid that lubricates the synovial membrane surfaces. This is why many joint products are focused on delivering more HA to the joints.
Joint cartilage also has another way of lubrication: with loading of weight on the joint, the fluid that sits between the cartilage cells gets squeezed out momentarily. Because opposing cartilage surfaces can make contact over about 10% of the total joint area, friction is decreased significantly by this lubricating mechanism. The quality of the cartilage (with its glucosaminoglycans, etc) will affect this lubrication process.
Osteo-arthritis
Osteo-arthritis (OA) is a disease that results from an interaction of a number of complex mechanisms. It can be caused by traumatic insults to the joint structures or by physiologic trauma. The end result is progressive deterioration of the joint cartilage and deleterious changes to the synovial membrane, which together result in bone-remodelling, pain, joint effusion and stiffness.
The equine athlete
It is well accepted that equine athletes carry an increased risk for development of OA. Healthy joint cartilage adjusts to the level of activity and weight-bearing. However, studies indicate that there is a limit to these adjustment capabilities, and activity beyond this point can result in maladjustment and injury of joint cartilage.
High-impact joint loading above this threshold has been shown to decrease cartilage proteoglycan content, increase levels of harmful enzymes (produced by the synovial membrane) and cause the death of chondrocytes (which are responsible for matrix production). Repeated high-impact activities can therefore decrease the quality of the joint cartilage over time, causing OA.
Joint support
There are many joint supplements on the market that contain various active constituents in different formulations and concentrations. Besides oral supplements, we also offer products that are injected in the muscle or vein, that have proven more effective. These products are especially suitable for horses that are still performing. In other words, some products are more effective than others and prices vary. Depending on your (horse’s) situation and goals, we can help you find a product that suits your demands.